He who has health has hope, and he who has hope has everything..
– Thomas Carlyle
Sub-Saharan Africa has 24 percent of the global disease burden, yet only three percent of the world’s health care workers..
– Mitchell Besser | HIV AIDS Activist
Community Health Services
The Palabora Foundation is invested in the health of people living in and around Phalaborwa. We help more than 1000 people per month from all communities in the Ba-Phalaborwa Municipality to access health services.
Community Health Services At A Glance
Phalaborwa, with an estimated population of 188 000, has more than 15 000 people that are on ARVs. This is only a fraction of people living with HIV and who have not started treatment. Given the burden of HIV in RSA and the fact that Phalaborwa is a mining area with many migrant labours, the number of clients on ARVs is too small. Nobody can prosper economically unless their primary health care needs are taken care of, which is why the Palabora Foundation is invested in the health of people living in and around Phalaborwa. In fact, the Palabora Foundation supports an average of 1300 people per month from all communities in the Ba-Phalaborwa municipality to access health services. Our flagship programs are:
HIV remains a key global public health issue and in South Africa about 8.2 million people are living with the virus. Ba-Phalaborwa municipality, has over 15 000 people living with HIV that are on ARV, has close to 9066 people that are on ARVs. We believe that there still people who are unaware of their HIV status or know their HIV status but are not yet on treatment. Our programme utilizes a system of education and programme monitoring to minimize the impact of HIV and to encourage people to test in order to access relevant treatment.
People on ARV's Phalaborwa (2024)

e empower the community through health education and information sharing so that they can better take care of their health. By being healthy the people will be in a position to go to school or work thereby contributing to the economy of the municipality.
Our interventions throughout the years have been sensitive to a call for evidence based programmes, and we have rallied behind the drive to focus on the most vulnerable groups, that is adolescent and young woman who are at increased risk to sexual exploitations resulting in unplanned pregnancies’.
Outreach services are also conducted at workplace, to give information to clients that in most cases are unable to visit health care facilities due to work and other commitments. This enables employees to access basic screening services without absenting themselves from work. It also helps health care professionals to discuss with employers on how to support employees that are on any chronic medications, without discriminating them.
Understanding Risk
Adolescents and young women are at an increased risk for HIV infection because of risky sexual behaviour. As a result, we focus on prevention of new HIV infections as well as finding better ways to engage these vulnerable groups so they can access relevant health services.
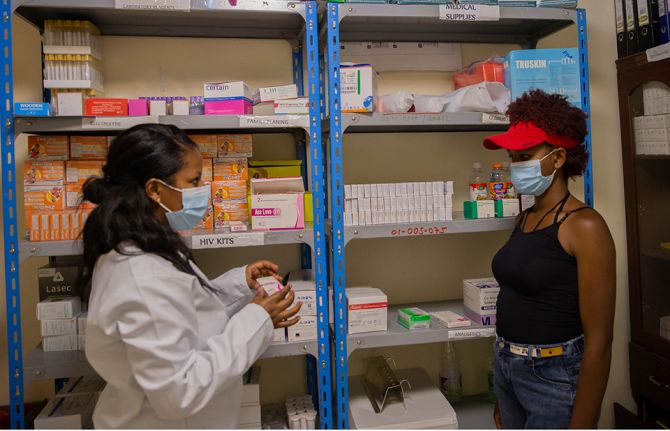
Impact of programmes on local communities
- We provide fast and efficient HIV and TB services. This means that clients that are working are able to come early in the morning for their monthly medication and still go to work on time. Time spent at the facility is less than 30 minutes as compared to government health facilities.
- We render consistent outreach services to schools, workplaces and churches.
- We have HIV ambassadors who openly advocates for the rights of people living with HIV in order to minimize stigma and discrimination.
- We have a good relationship with Traditional Health Practitioners (THPs). This ensures that clients that are in their care are not prevented from taking their chronic medications whilst in the care of THPs.
- Adherence Clubs are established, where stable clients are grouped together and receive two months supply of treatment without having to queue. We have already established 13 clubs as a way of aligning ourselves with the national guidelines. The current HIV policy, Universal Test and Treat (UTT) stipulates that we must test and initiate treatment to those that test positive within 3days is adhered to.
- We make a difference in peoples lives by encouraging them to embrace their HIV status without fear of stigma and discrimination
- There is a decreased number of lost – to – follow up clients on ARVs and TB treatment as a result of the tracking and tracing of treatment defaulters conducted.
Our work has attracted the attention of the American embassy’s PEPFAR. As a result of these initiatives, in 2016 – 2017 PEPFAR awarded us a grant to conduct youth dialogues at high schools, TVET colleges and Drop in centres.
Outreach Services
hose who test positive for HIV are provided with continuous counselling on how to live a positive and productive lifestyle, but our outreach services extend well beyond this. One of the National strategic goals is to have an HIV free generation by 2030. As a result outreach services are conducted as a way of reaching out to people who due to their employment, are unable to visit health facilities for basic screening purposes. Outreach services are also conducted at schools where there are vulnerable groups. This is aimed at preventing new infections amongst teenagers and young adults by engaging them through health dialogues.
We visit workplaces and conduct HIV counselling and testing, basic screening for TB, Blood Pressure and Diabetes Mellitus on site. Clients that are tested positive for any disease are referred to health facilities of their choice for comprehensive treatment, care and management.
We also visit schools to give health information and education to learners in the environment where they already congregate and feel comfortable to interact with health workers and to ask questions.
We want to serve all community members that have limited or no access to health care facilities because of them being unable to get or negotiate time off from their employment without money being deducted from their salaries.
These efforts add to what the local Department of Health is providing and we receive all medications and other pharmaceutical supplies from them.
WE VISIT BOTH PRIMARY AND HIGH SCHOOLS AS LONG AS THEY GIVE US PERMISSION TO DO SO. THERE ARE 31 PRIMARY SCHOOLS AND 13 HIGH SCHOOLS THAT WE ENGAGE.

Challenges include the limited time we have to interact with employees. We are usually allowed to utilise lunch time for both information giving and screening. At schools the challenge is also the time allocated, which is very limited to two a maximum of two periods, with more than 100 pupils in attendance. Attending to a large number of youngsters at a time poses challenges of poor concentration span for some pupils.

Household Visits
his work also aligns with one of the National strategic goals, where 95% of clients that are on ARVs are to be kept in care or in the programme.
The surrounding clinics submit their lists of newly initiated clients and Lost to follow up (LFTU) clients to our monitoring team on monthly basis. The team then track and trace the clients, provide treatment adherence counselling and bring them back in care, provided they are willing to continue with treatment.
Firstly we conduct household visits to clients who are newly initiated on treatment (ARV or TB Treatment) to monitor if they are experiencing side effects that may contribute in clients discontinuing the treatment.
Secondly we make follow up visits to clients who miss their appointment dates for treatment collection. Depending on the reason for missing the appointment date, the client’s family is encouraged to come to the facility to collect the treatment on behalf of the client.
The support mainly consists of counselling. Since we are using People Living with HIV (PLWH) as our monitoring team, it becomes easier for clients to relate and voice out their fears, concerns and challenges. Some clients give wrong residential addresses or relocate to other places without reporting to the health facilities, thereby making it difficult to locate them, but on the whole, this programme is very successful.
Youth Dialogue
Teenagers and young adults are currently the most vulnerable groups when it comes to HIV infection because of engaging in risky sexual behaviours like having multiple sexual partners without using protection and having unprotected sexual intercourse with older persons for nancial gain or due to peer pressure.
The youth dialogues are meant to conscientise these vulnerable groups about the benefits of remaining healthy. We use dialogues because young people tend to participate more actively and freely when they are amongst their peers.
Condom Distribution
Prevention is better than cure. Condoms are distributed to High Transmission Areas like taverns, where patrons are likely to engage in risky sexual behaviours which will predispose them to STI’s. We also conduct demonstrations to ensure people know how to use the condoms.
We are a primary condom distributor because the facility has condom storage rooms that meet the DoH national standards. We therefore receive up to 600 000 male condoms and 10 000 femidoms in one delivery, from the national office, for distribution to the local hospital, clinics, surrounding mines, high transmission areas and workplaces.
WE GIVE OUT 130000 MALE CONDOMS AND 2000 FEMIDOMS PER MONTH!
Who We Work With
DEPARTMENT OF HEALTH (DOH) We get all the pharmaceutical supplies, including medication from the local hospital. Difficult and unstable clients are referred for specialist consultation and management. Professional nurses, Data Capture and Lay Counsellors are capacitated when new developments are introduced in the programme.
DEPARTMENT OF EDUCATION (DOE) grants us access to school children during school hours to conduct health dialogues.
DEPARTMENT OF SOCIAL DEVELOPMENT we refer qualifying clients to access food parcels and relevant social grants.
BA-PHALABORWA MUNICIPALITY assist with community mobilization during health events/ campaigns.
PHALABORWA FM helps us to market our services and mobilise our community.
HLOKOMELA helps us with condom logistics management and condom distribution in high transmission areas.


